Artificial Intelligence Applications in Healthcare for Early Disease Diagnosis: Revolutionizing Predictive Health
The landscape of modern medicine is undergoing a profound transformation, driven by the exponential growth of data and the remarkable capabilities of artificial intelligence. At the forefront of this revolution is the burgeoning field of artificial intelligence applications in healthcare for early disease diagnosis. This pivotal area promises to shift the paradigm from reactive treatment to proactive, preventative care, offering unprecedented opportunities to detect illnesses at their most treatable stages. As an SEO expert, I understand the critical importance of not just covering this topic comprehensively, but also doing so in a way that resonates with search intent, provides immense value, and establishes authoritative expertise. Prepare to delve into how AI is becoming an indispensable ally in the quest for earlier, more accurate, and ultimately, life-saving diagnoses.
The Imperative of Early Disease Diagnosis in Modern Healthcare
The adage "prevention is better than cure" holds profound truth in healthcare, yet often, by the time symptoms manifest, diseases have progressed significantly, making treatment more challenging, invasive, and costly. Early disease diagnosis is not merely beneficial; it is critical for improving patient outcomes, reducing mortality rates, and alleviating the immense burden on healthcare systems. Traditional diagnostic methods, while foundational, often face limitations such as reliance on subjective interpretation, time-consuming lab processes, and the sheer volume of data that human clinicians must process. This is where the power of artificial intelligence steps in, offering capabilities that far surpass human limitations in terms of speed, scale, and pattern recognition.
Limitations of Traditional Diagnostic Approaches
- Subjectivity: Human interpretation, particularly in image analysis (radiology, pathology), can vary between experts.
- Data Overload: Clinicians are inundated with vast amounts of patient data, from electronic health records (EHRs) to genomic sequences, making it difficult to identify subtle patterns indicative of early disease.
- Time Constraints: Manual analysis of complex data sets is time-consuming, delaying diagnosis and intervention.
- Reactive Nature: Many traditional methods are applied after symptoms appear, rather than proactively identifying risk.
How AI Revolutionizes Early Detection: A Paradigm Shift
Artificial intelligence, particularly its subfields of machine learning algorithms and deep learning, excels at processing, analyzing, and interpreting massive datasets with unparalleled speed and precision. This ability is fundamentally reshaping how we approach early disease diagnosis, moving from a reactive model to a highly proactive, predictive analytics framework. AI systems can identify intricate patterns and correlations in data that are imperceptible to the human eye, enabling the detection of subtle early indicators of disease long before overt symptoms appear.
AI in Medical Imaging Analysis: Unveiling Hidden Clues
One of the most impactful artificial intelligence applications in healthcare for early disease diagnosis is in medical imaging. AI-powered tools can analyze X-rays, CT scans, MRIs, ultrasounds, and even microscopic pathology slides with incredible accuracy and speed. These systems are trained on vast datasets of annotated images, learning to identify anomalies, lesions, and subtle changes that might indicate early-stage diseases like cancer, neurological disorders, or cardiovascular conditions.
- Radiology: AI algorithms can assist radiologists in detecting lung nodules (early signs of lung cancer), breast lesions in mammograms, or subtle changes indicative of stroke on brain scans. This significantly improves diagnostic accuracy and reduces false negatives. Explore more about AI in radiology.
- Pathology: Analyzing digital pathology slides, AI can automatically identify and quantify cancer cells, grade tumor aggressiveness, and detect rare cellular abnormalities, supporting pathologists in making quicker and more consistent diagnoses.
- Ophthalmology: AI is proving invaluable in screening for diabetic retinopathy, glaucoma, and macular degeneration from retinal scans, enabling early intervention to prevent vision loss.
Leveraging Genomic and Proteomic Data for Personalized Risk Assessment
The era of precision medicine is here, and AI is its backbone. By analyzing complex genomic, proteomic, and metabolomic data, AI can identify genetic predispositions to certain diseases, predict individual drug responses, and uncover novel biomarker discovery for early disease indicators. This allows for highly personalized risk assessments and tailored preventative strategies.
- Genetic Risk Prediction: AI models can sift through vast genomic databases to identify gene variations associated with increased risk for conditions like certain cancers, heart disease, or Alzheimer's, years before onset.
- Drug Response Prediction: Understanding how an individual's genetic makeup influences their response to medication can optimize treatment plans and reduce adverse effects.
- Biomarker Identification: AI algorithms can discover new biomarkers (measurable indicators of a biological state) in blood, urine, or tissue samples, which can signal the presence of disease at its earliest stages.
Wearable Devices and Continuous Monitoring: Proactive Health Surveillance
The proliferation of wearable health devices (smartwatches, fitness trackers, smart patches) generates continuous streams of physiological data. AI is crucial for transforming this raw data into actionable insights for preventative care and early disease detection. By monitoring heart rate, sleep patterns, activity levels, blood oxygen, and even ECG readings, AI can detect subtle deviations from an individual's baseline, signaling potential health issues.
- Anomaly Detection: AI algorithms can learn an individual's normal physiological patterns and flag unusual changes (e.g., sudden heart rate variability, prolonged sleep disturbances) that might indicate the onset of conditions like arrhythmias, infections, or even stress-related issues.
- Real-time Alerts: Systems can issue proactive alerts to users or their healthcare providers if concerning patterns emerge, prompting timely medical evaluation.
- Chronic Disease Management: For individuals with chronic conditions like diabetes or hypertension, continuous monitoring combined with AI can help manage the disease, predict exacerbations, and prevent complications.
AI-Powered Clinical Decision Support Systems (CDSS): Empowering Clinicians
AI is not designed to replace clinicians but to augment their capabilities. Clinical decision support systems, powered by AI, integrate and analyze diverse patient data – from EHRs, lab results, medical images, and even external research – to provide evidence-based recommendations and insights to healthcare professionals. These systems can highlight potential diagnoses, suggest appropriate tests, and flag medication interactions, significantly enhancing diagnostic accuracy.
- Diagnostic Assistance: AI can process complex patient histories and symptoms, cross-referencing them with vast medical knowledge bases to suggest a list of differential diagnoses, helping clinicians avoid diagnostic errors.
- Risk Stratification: By analyzing a patient's entire health profile, AI can stratify their risk for developing certain conditions, guiding more targeted screening and preventative interventions.
- Information Synthesis: In the age of information overload, CDSS can quickly synthesize relevant research and guidelines, ensuring clinicians have access to the latest evidence at the point of care. This integrates seamlessly with health informatics principles.
The Mechanics: AI Technologies Driving Early Diagnosis
Understanding the underlying AI technologies is key to appreciating their transformative potential. The primary drivers are machine learning, deep learning, natural language processing, and computer vision.
Machine Learning and Deep Learning in Healthcare Data Analysis
At the core of most AI applications for early diagnosis are machine learning algorithms. These algorithms are trained on vast amounts of data to identify patterns and make predictions without being explicitly programmed for each task. Deep learning, a subset of machine learning, utilizes neural networks with multiple layers to learn complex representations from data, making it particularly effective for image and unstructured data analysis.
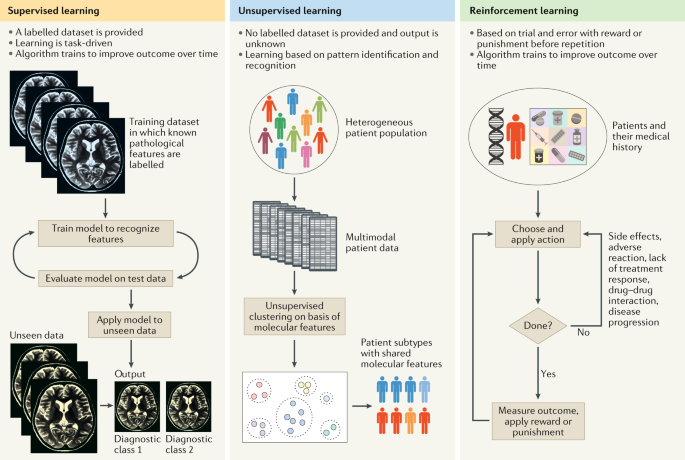
- Supervised Learning: Used for tasks where the AI is trained on labeled data (e.g., images labeled as "cancerous" or "non-cancerous") to classify new, unseen data. This is crucial for medical imaging.
- Unsupervised Learning: Employed to find hidden patterns or clusters in unlabeled data, useful for discovering new disease subtypes or identifying novel biomarkers.
- Reinforcement Learning: While less common in direct diagnosis, it can be used in optimizing treatment pathways or managing patient flow based on learned outcomes.
Natural Language Processing (NLP) for Unstructured Data
A significant portion of clinical data exists in unstructured formats, such as doctor's notes, discharge summaries, and patient narratives. Natural Language Processing (NLP) enables AI systems to understand, interpret, and extract meaningful information from this text-based data. NLP can identify subtle symptoms mentioned in notes, flag family histories of disease, or even detect emotional cues that might indicate mental health issues, all contributing to a more holistic diagnostic picture.
Computer Vision for Visual Diagnostics
Computer Vision is the field of AI that enables computers to "see" and interpret visual information. This technology underpins the success of AI in medical imaging analysis, allowing systems to detect abnormalities, measure structures, and quantify disease progression directly from images, often with greater consistency than human observers.
Benefits Beyond Detection: Enhancing Patient Outcomes and Healthcare Efficiency
The impact of artificial intelligence applications in healthcare for early disease diagnosis extends far beyond simply identifying illnesses. The ultimate goal is to enhance overall patient outcomes and optimize the efficiency of healthcare delivery.
- Improved Treatment Efficacy: Diagnosing diseases earlier means interventions can begin when they are most effective, often leading to less aggressive treatments, better recovery rates, and reduced risk of complications.
- Reduced Healthcare Costs: Early diagnosis can significantly lower the long-term cost of care by preventing disease progression that would require expensive, intensive treatments or long-term management. Preventative care is inherently more cost-effective.
- Empowered Patients: Receiving an early diagnosis allows patients and their families more time to understand their condition, explore treatment options, and make informed decisions, reducing anxiety and improving quality of life.
- Optimized Resource Allocation: By identifying high-risk individuals, healthcare systems can allocate resources more efficiently, focusing screening and preventative efforts where they are most needed.
Challenges and Ethical Considerations in AI for Early Diagnosis
While the promise of AI in early disease diagnosis is immense, its implementation is not without challenges. Addressing these concerns is crucial for widespread adoption and public trust.
- Data Privacy and Security: AI systems require access to vast amounts of sensitive patient data. Ensuring robust data security and adhering to privacy regulations (like HIPAA and GDPR) is paramount.
- Algorithmic Bias: If AI models are trained on biased datasets (e.g., predominantly from one demographic group), they may perform poorly or inaccurately for underrepresented populations, leading to health disparities.
- Regulatory Hurdles and Validation: AI diagnostic tools must undergo rigorous testing and validation to prove their safety, efficacy, and reliability before widespread clinical use. Regulatory bodies are still developing frameworks for these technologies.
- Integration into Workflow: Seamlessly integrating AI tools into existing clinical workflows and electronic health records systems can be complex.
- Human Oversight and Trust: Clinicians need to understand how AI tools arrive at their conclusions (interpretability) and maintain ultimate responsibility for diagnostic decisions. Building trust in AI recommendations is key.
Practical Steps for Healthcare Providers Embracing AI for Early Diagnosis
For healthcare organizations looking to leverage the power of AI for early disease detection, a strategic approach is essential:
- Invest in Robust Data Infrastructure: AI thrives on high-quality, well-organized data. Healthcare providers must prioritize secure, interoperable electronic health record (EHR) systems and data warehousing solutions.
- Foster Collaboration: Partner with AI technology developers, academic institutions, and data scientists. This cross-disciplinary collaboration is vital for developing and validating effective AI solutions.
- Prioritize Data Governance and Ethics: Establish clear policies for data collection, storage, usage, and sharing. Implement ethical guidelines to ensure fairness, transparency, and accountability in AI applications.
- Train Healthcare Professionals: Educate clinicians, radiologists, pathologists, and other staff on how to interact with AI tools, interpret their outputs, and understand their limitations. AI literacy is crucial.
- Start with Pilot Programs: Begin with small-scale pilot projects focusing on specific diseases or diagnostic pathways where AI can demonstrate clear value, then scale up based on success.
- Focus on Clinical Validation: Ensure that any AI diagnostic tool undergoes rigorous clinical validation with diverse patient populations to prove its real-world effectiveness and safety.
By taking these actionable steps, healthcare providers can confidently navigate the integration of AI, harnessing its potential to deliver superior diagnostic accuracy and improve patient outcomes across the board.
The Future Landscape: AI and Predictive Health
The journey of artificial intelligence applications in healthcare for early disease diagnosis is just beginning. As AI technologies continue to mature, we can anticipate even more sophisticated predictive models, capable of integrating data from an even wider array of sources – environmental factors, social determinants of health, and continuous physiological monitoring – to create truly holistic and dynamic health profiles. The future of healthcare is undeniably moving towards a proactive, individualized model where AI serves as the intelligent backbone, ensuring that diseases are not just treated, but often prevented, or caught at their earliest, most curable stages. This evolution promises a healthier future for all, underpinned by advanced health informatics and intelligent systems.
Frequently Asked Questions
What specific diseases can AI help diagnose early?
AI is showing immense promise in the early diagnosis of a wide range of diseases. In oncology, it's used for early detection of various cancers (lung, breast, prostate, skin, colorectal) through medical imaging and genetic analysis. For cardiovascular diseases, AI can identify early signs of heart failure, arrhythmias, and coronary artery disease from ECGs, wearable data, and imaging. In neurology, it aids in the early detection of Alzheimer's, Parkinson's, and stroke. AI also contributes to diagnosing conditions like diabetic retinopathy, glaucoma, and certain infectious diseases or sepsis at their initial stages, significantly improving patient outcomes.
Is AI meant to replace doctors in diagnosis?
No, AI is not intended to replace doctors but to augment their capabilities. AI tools are powerful assistants, providing clinicians with enhanced analytical power, faster data processing, and access to vast medical knowledge. They can highlight subtle patterns, prioritize cases, and offer evidence-based insights, thereby improving diagnostic accuracy and efficiency. The final diagnostic decision and patient care responsibility always remain with the human clinician, who brings empathy, ethical judgment, and the ability to handle complex, nuanced patient situations that AI cannot replicate.
How accurate are AI diagnostic tools?
The accuracy of AI diagnostic tools varies depending on the specific application, the quality of the training data, and the complexity of the disease. In many areas, particularly in medical imaging analysis, AI systems have demonstrated accuracy comparable to, or even exceeding, that of human experts for specific tasks, especially in identifying subtle anomalies. For instance, some AI algorithms for diabetic retinopathy detection have achieved very high sensitivity and specificity. However, it's crucial that these tools are rigorously validated in real-world clinical settings and continuously refined to ensure their reliability and fairness across diverse patient populations, contributing to improved diagnostic accuracy overall.
What are the main challenges in implementing AI for early diagnosis?
Implementing AI for early disease diagnosis faces several key challenges. Firstly, ensuring data privacy and security is paramount, given the sensitive nature of health information. Secondly, addressing algorithmic bias, where AI models might perform poorly on underrepresented groups due to biased training data, is critical for equitable healthcare. Thirdly, navigating complex regulatory frameworks and obtaining clinical validation for AI tools can be time-consuming. Finally, integrating AI seamlessly into existing healthcare workflows and fostering trust among clinicians and patients requires significant effort in training and change management, alongside robust health informatics infrastructure.
How does AI handle patient data privacy?
Handling patient data privacy is a top priority for AI applications in healthcare. Robust measures are employed, including data anonymization and de-identification, where personal identifiers are removed from datasets used for training AI models. Secure data storage and transmission protocols, such as encryption, are standard practice. Compliance with strict regulatory frameworks like HIPAA in the U.S. and GDPR in Europe is mandatory. Furthermore, emerging technologies like federated learning allow AI models to be trained on decentralized datasets without the raw data ever leaving the healthcare institution, significantly enhancing privacy and contributing to ethical data analysis practices.

0 Komentar